The Justin Curran, DO, FACOEP Story
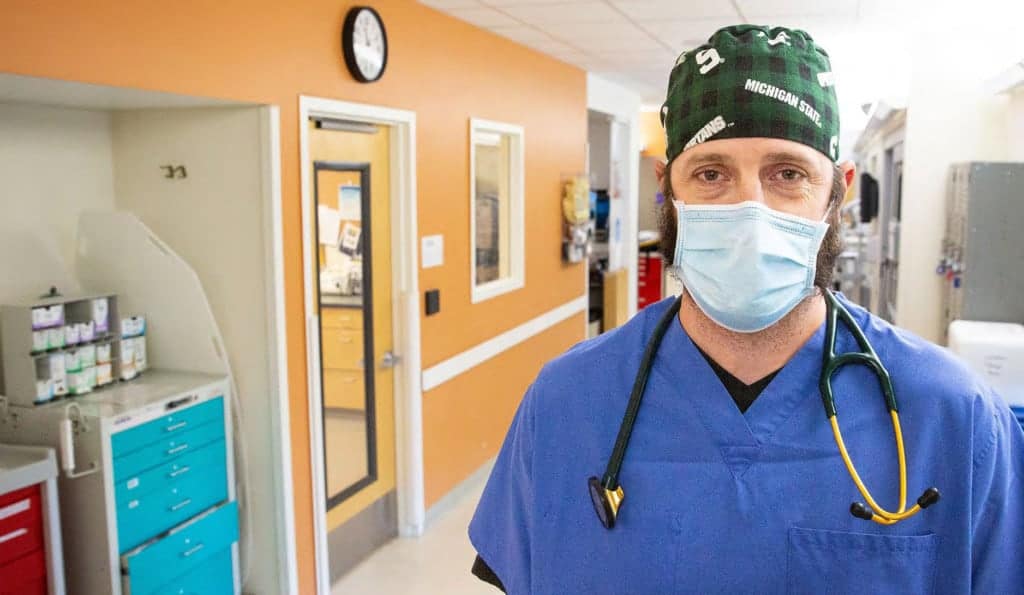
Department: Emergency Department
Courage Is Multi-Faceted In The Emergency Department
What makes working in the Emergency Department (ED) at Island Hospital rewarding is exactly what makes it challenging. Even before the pandemic, ED staff had to diagnose and treat a variety of medical issues in multiple patients simultaneously. COVID-19 added complicating layers to an already intense environment.
Justin Curran, DO, FACOEP, has worked in the ED since 2011 and loves the variety, intensity and pace of the job. “The most rewarding part is helping people through a variety of situations,” Curran said. “We can go from one room where someone is having a heart attack, to a patient with respiratory failure from COVID, to a broken hip, to a kidney infection with sepsis, to a child with a runny nose.”
Knowing where each patient is in the course of their evaluation, bouncing from room to room (12 total with four hall carts and a triage room) and fielding calls from cardiologists, orthopedists, general surgeons, pediatricians and other specialists is all part of the job. Curran and his staff work hard to make sure expectations are met.
“Our goal is to rapidly and accurately assess, treat and stabilize everything that comes our way,” he said. “When COVID-19 hit, it was outrageously difficult,” explained Curran. “In the beginning, staff were scared and stressed, afraid of transmitting the virus to their families. And while patient volumes dropped, those who did come in were much sicker. Now that the ED and hospital have standard treatment algorithms, the biggest challenge is staff fatigue. We are spent. We are exhausted.”
Twenty percent of the healthcare work force has either retired or left the profession for less risky work, and hospitals have been at or over capacity during several peaks of the pandemic. Despite the heavy lifting being asked of him, Curran expects to be here doing his work for a long time.
JUSTIN CURRAN, DO, FACOEP, is a residency-trained emergency medicine physician. He graduated from Michigan State University Medical School in 2007 and completed his four year residency at POH Regional Medical Center (now McLaren Oakland), where he served as chief resident his final year. Just prior to coming to Anacortes in 2011, he was a flight physician for AeroMed.
Island Hospital
Emergency Department
islandhealth.org/ed
360.299.1300
